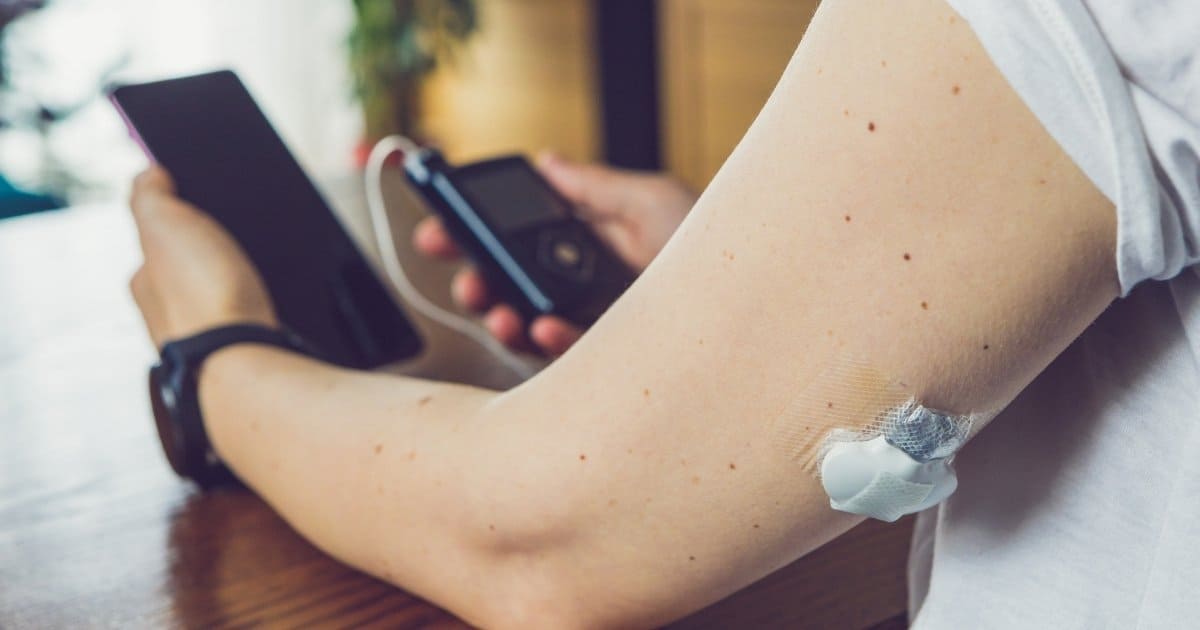
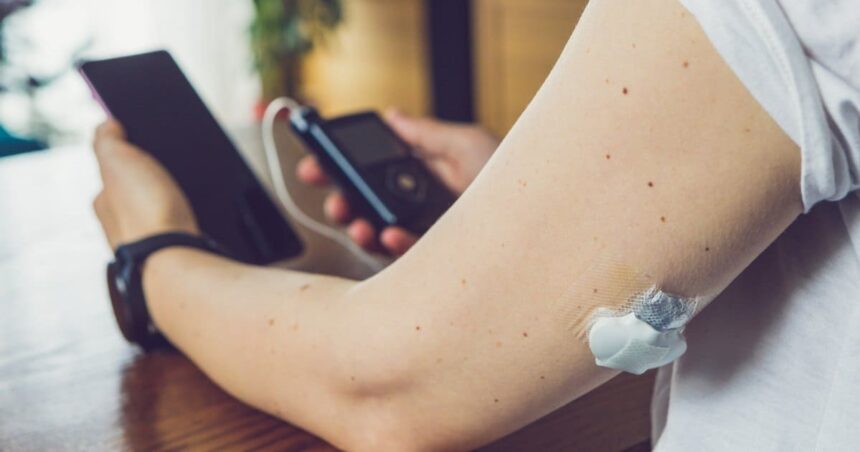
If you have recently changed from multiple daily injections (MDIs) to insulin pump therapy, changes in treatment can be overwhelming and confusing.
Many aspects of daily life need to be changed, such as what kind of insulin you can take.
Not all types of insulin work with an insulin pump, so caution should be taken when making changes. In this article, we will investigate which types of insulin are suitable for insulin pump therapy and which types are not.
Always advise your doctor before making any changes to your treatment, especially if you are switching from MDI to insulin pump therapy.
How does insulin pump therapy work?
Insulin pump therapy works by allowing patients to be given continuously and continuously under the skin in an injection set that operates remotely from the Insulin Manager (PDM) or an insulin pump, instead of taking insulin injections manually on everything they eat (and one or two “long-acting” insulin injections).
Intravenous insulin acts as basal insulin, so it is usually used for both basal and bolus administration of insulin, which usually acts rapidly.
What types of insulin can be used with an insulin pump?
no. It is important to work with your doctor to determine which insulin is best for you with an insulin pump, but strictly speaking, only fast acting insulins such as Aspert (Novolog and Fiasp), Lispro (Humalog and Lyumjev), and Glulisine (Apidra) can be safely used with insulin pumps.
The two latest (and fastest) insulins are fiasp and lyumjev, which become anecdotally effective within 5 minutes of administering them. They are both approved for use with insulin pumps and are a great choice if you are struggling to blend in beforehand for your meal (you can even ingest it) rear Eat meals, especially if you’re eating low/low carbs. )
Note: FIASP is currently not recommended for tandem T-SLIM pumps as Tandem has not conducted any research to verify safety and efficacy in its systems..
Normal insulins such as humulin and novoline R are no longer commonly used (except for some medical circumstances, sometimes with type 1 diabetes patients and type 2 diabetes who maintain a strict ketonogenic diet), but they may be used with insulin pumps, but are not always recommended.
Fast acting insulin in the insulin pump is more suitable due to the mechanism by which insulin is continuously distributed.
This continuous basal velocity replaces the need for long-acting insulin shots such as Glargine (Lantus, Basaglar, and Toujeo), Detemir (Levemir), or Degludec (Tresiba).
The effectiveness of long-acting insulin is intentionally delayed, so this causes a disaster if patients are given to insulin pumps without taking insulin immediately, causing a serious blood glucose collision later in the day.
The types of insulin available to insulin pumps are further determined by insurance coverage, what your doctor prescribes, and your preferences.
The guide will help you learn more about the different types of insulin.Insulin Type: Peak and Period”.
Why use only rapid insulin?
In short, fast acting insulin achieves better blood sugar levels and provides better patient control than using pump-acting insulin.
The advantage of working insulin quickly is that they are effective immediately. Usually, the peak reaches approximately 1 hour within 10-15 minutes of administration.
The total duration of rapidly acting insulin in the body is 3-4 hours, depending on your metabolism and ability to process insulin.
Furthermore, while using insulin, which acts rapidly with an insulin pump, you can better manage your hyperglycemia levels, attempting to manage your blood glucose levels with insulin alone is both cumbersome and dangerous due to delayed effects, multiple peaks, and length within the body.
Can you remove long-acting insulin forever?
In theory, yes, but having a prescription for long-acting insulin in your hand is always helpful (and, if possible, some spare vials of insulin that will act long-act on the fridge!).
Insulin pumps, like all technologies, can break down from time to time, and it’s helpful to have insulin if something goes wrong and have a backup mechanism to manage diabetes.
If the insulin pump breaks, it can take several days to get the manufacturer to ship a new one. You may also not want to wake up all night to get a minibolus of fast acting insulin (once or twice a day, instead of long-acting shots!).
Ask your doctor to prep prescriptions for Glargine (Lantus, Basaglar, and Toujeo), Detemir (Levemir), or Degludec (Tresiba). Therefore, if necessary, multiple daily injections (MDIs) can be relied on if necessary without too much disruption to the diabetes manager.
You may also want to “break” your insulin pump from time to time. Those who are very active in the summer, who want to play many water sports or swim in the pool or the ocean without worrying about injection sites, can also take a break from the patch or tube and return to manual injection.
Having some spare long-acting insulin nearby can help. Or even if you’re just burned out from insulin pump therapy in general.
Read more about potential issues with taking insulin.Side effects of insulin: Things you need to know”.
Are there any drawbacks to using only rapid action insulin?
Although there are not many drawbacks to using only insulin, which acts rapidly insulin pumps, it increases the risk of developing hyperglycemia and the risk of developing diabetic ketosidosis (DKA).
This is due to the mechanism by which insulin acts rapidly and the fact that it is completely removed from the system within 3-4 hours.
Overnight insulin pump malfunctions, diabetics may not have active insulin in their bodies for hours, which is dangerous.
People who ride an MDI and take both fast and long-acting insulin, always maintain a backstop of long-acting insulin in their system (most often) to prevent the onset of DKA.
Furthermore, if you forget to have a bolus for your diet, you may experience higher blood sugar levels as a result of not having insulin, which also acts long-term in the body as a backstop.
You are using an insulin pump by riding an insulin pump that is exclusively equipped with insulin and using multiple daily injections (MDIs) that are mixed with long-acting insulin, so it’s up to you to make the best choice for you and your diabetes (under guidance from a doctor).
You can read the article “Why choose multiple daily injections over insulin pumps” Learn more about the pros and cons of MDI and insulin pumps.
Conclusion
Insulin pumps are an incredible part of diabetes technology that works by releasing small amounts of insulin regularly throughout the day with continuous infusions, as the natural pancreas does for people without diabetes.
This small amount of insulin, distributed by an insulin pump, is called basal velocity and is different for everyone.
You need to work with your doctor to determine the basic rate and bolus structure that is suitable for you, your diet, your goals, and your lifestyle.
However, certain things are constant. Only fast acting insulin (and sometimes regular insulin) considered suitable for insulin pumps are considered.
This is because continuous infusions of rapidly acting insulin replace the need for long-acting insulin injections once a day. That same rapid insulin also acts as a bolus insulin administered by a patient to the insulin pump.
Rapidly acting insulin at insulin pumps is used for both basal and underlying purposes and requires long-acting injections.
This may all sound confusing at first, but in reality it makes life easier for people with diabetes.
You can learn more about insulin therapy in these articles.