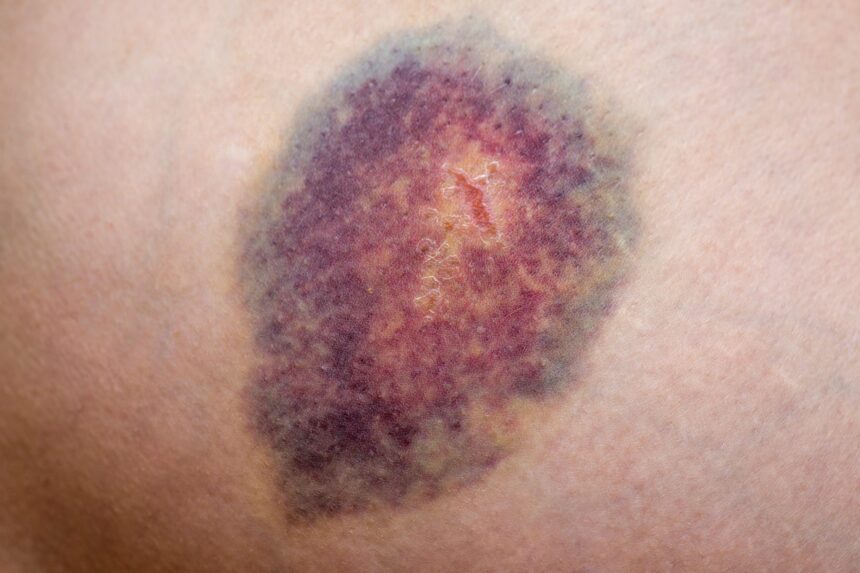
Shutterstock
If you have diabetes and your skin feels like a bruise too easily, it may not be your imagination. One of the minor side effects of diabetes (both type 1 and type 2) is the tendency for bruises to form easily and slowly soothe.
Bruises are usually not a serious problem, but can be a bad sign for your overall health. Like diabetes, the perpetrator is hyperglycemia.
What exactly is the bruise?
Bruises – The technical term for bruising occurs when blood vessels under the skin leak into surrounding tissue. Bruises can appear yellow, blue, red, purple, or black, and change color over time as they heal. They may or may not be painful.
Bruises can look rather ugly, but most of the time they are not a big deal and they heal themselves. However, there are exceptions if the bruise requires a doctor’s appointment.
The term hematoma is used to describe more serious levels of bruise. At this level, there is enough coagulation blood to give the skin a raised or lumpy sensation. Hematomas can be the result of more serious injuries and may require the help of a doctor to heal properly.
Diabetes and simple bruises
Diabetes does not cause bruises without explanation, but it can make bruises more easily from common injuries and slow the bruise process.
Like most diabetic complications, enhanced bruises are ultimately caused by increased chronic hyperglycemia levels, leading to problems with blood flow and delayed wound healing. Blood circulation disorders in diabetic patients inhibit the flow of oxygen, nutrients and immune cells to the wound. Diabetes is also associated with abnormal blood clotting, vascular dysfunction, and imbalances in collagen formation, resulting in a stiff and flexible skin. All of these unfortunate effects may contribute to simple bruises.
Bruises are not generally considered serious, but in rare cases, bruises may require medical consultation. Consider this anecdote from the Massachusetts hospital network. In this network, a longtime type 1 diabetic woman bumps shin with a bike pedal, and the bruises don’t heal itself. She ended up needing months of care for it. In the worst case scenario, a nonhealing wound can ultimately lead to an amputation.
Diabetic bruising
Furthermore, diabetes can be more likely to cause certain types of bruises to begin with. If you have neuropathy and your limb senses are reduced, you may be more likely to hit them on a heavy object. A common problem is foot injuries. If you don’t notice that your shoes have pebbles because your feet have lost so many feelings, you can cause damage without knowledge.
Syringes used for injectable drugs such as Ozempic that contain insulin and GLP-1 receptor agonists can also cause bruises just like the lancets that the lancets require to measure blood glucose in the fingers. These bruises are less likely to occur when you use brand new sharp needles each time and do not press too hard. Insulin pumps and continuous glucose monitors can also cause bruises.
Frequent bruises from needles can help to cause the formation of fatty masses under the skin that interfere with drug absorption. More quickly, they may cause embarrassment.
Other causes of simple bruises
Diabetes is not the only cause of simple bruises. The Cleveland Clinic shows some of the other potential perpetrators.
- Elderly (skinned and less blood vessels provide protection)
- Many drugs including nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and corticosteroids
- A simple family history of bruising
- Several dietary supplements including ginkgo biloba
- Blood disorders such as hemophilia
- Vitamin C or K deficiency
How to treat bruising
Most bruises take care of themselves, but a little first aid may help accelerate the healing process.
- Rest and raise the injured area to reduce blood flow to bruises and limit bleeding.
- Apply ice to slow blood flow and reduce swelling and pain.
- To reduce swelling, wear a light bandage around the bruise.
When should I call the doctor?
Bruises usually do not require medical attention, but bruising that do not occur or that usually does not heal may require testing. If you have experience, you may want to meet a healthcare provider.
- Bruise of unknown cause
- Repeated banging
- A bruise that doesn’t seem to heal
- An abnormally painful or rough bruise (hematoma)
Diabetes and other skin problems
A variety of unrelated skin problems are common in both type 1 and type 2 diabetes. People with diabetes are more likely to experience both common skin problems, such as dry skin and fungal infections, as well as more specific conditions, such as “shin spots” and diabetic dermatosis.
The skin is the largest organ in the body, and many of its blood vessels and nerves experience dysfunction when they receive hyperglycemia, just like the rest of the body. Even harmless skin problems are considered as warning signs that hyperglycemia must be addressed before they lead to more serious problems, such as heart and kidney health complications.
Take home
Diabetes, which impairs blood circulation and wound healing, can be slower in easy bruises and bruising. Optimal blood glucose control can be helpful in order to protect your body from injuries in the first place.
Bruises are usually not serious, but in rare cases, you may need to see a doctor. A simple bruise could be a warning sign that you are already experiencing a measure of hyperglycemia that can cause other more dangerous complications. Pay attention to bruises and let your health care provider know if there are any mystically developed bruises or anything that appears to be unhealed.
(TagstoTranslate) Bruises (T) Diabetic complications (T) Fat hypertrophy (T) Needle (T) Skin care (T) Skin disease